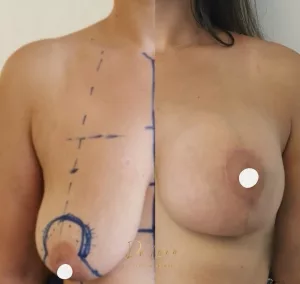
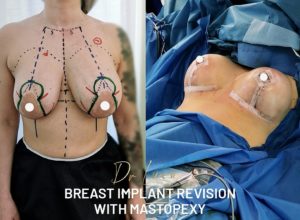
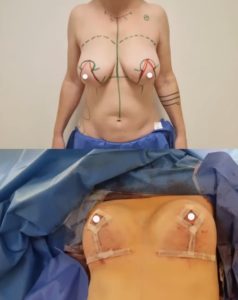
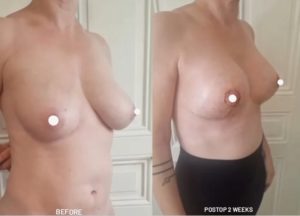
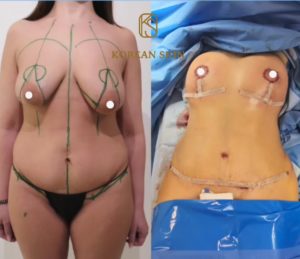
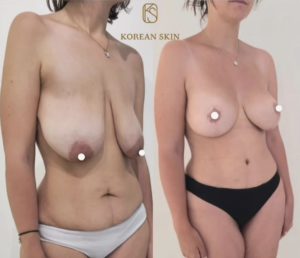
Ideal anatomy and proportion:
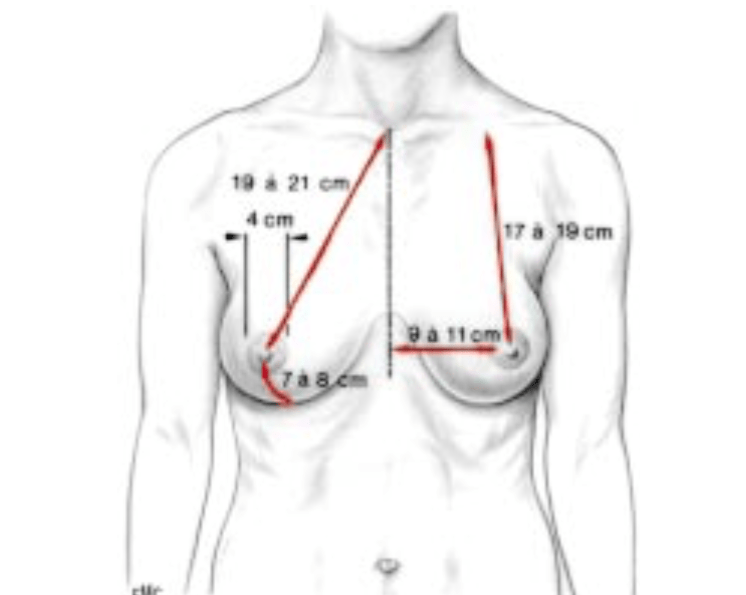
The ideal breast is 10-12 cm wide and the 2 nipples are about 20 cm apart (variable according to thorax width and patient morphology). The areola, with an ideal diameter of 38-45 mm, should be located 20 cm from the top of the sternum or halfway between the shoulder (acromion) and the elbow (epicondyle) and the distance between the nipple and the submammary fold should be about 7 cm.
Breast ptosis
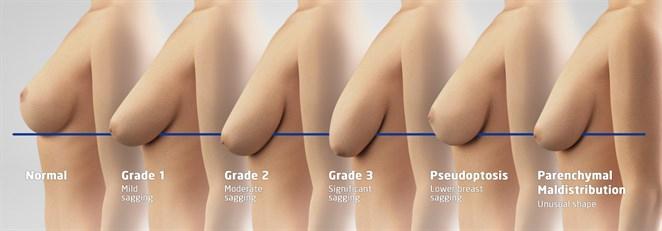
Over time, after a change in weight, pregnancy or breastfeeding, the breast tends to sag (ptosis) and the cleavage becomes empty. Mastopexy, or breast lift, allows the breast to be lifted, while filling the décolleté.
The areola should ideally be located halfway up the arm or 2-3 cm above the submammary fold (Pitanguy’s point) and most of the breast volume should be above the horizontal line corresponding to the submammary fold:
- If the nipple is at the level of the submammary fold, it is called type I (minimal) ptosis
- If the nipple is 1 to 3 cm below the submammary fold, it is called type II ptosis (moderate)
- If the nipple is more than 3 cm below the breast fold, it is called type III ptosis (severe)
- If the nipple is at the right height, but most of the volume of the breast is located under the submammary fold, then it is called pseudoptosis
Technique
The degree of ptosis determines the choice of technique.
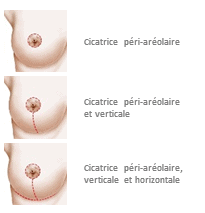
In fact, in grades II and III, a breast lift with inverted T scars is essential. In grade I, a breast lift with a peri-areolar scar (around the areola) +/- vertical scar may be sufficient. To treat pseudoptosis, a horizontal scar in the submammary fold may be sufficient in some cases. When the neckline (upper-internal part of the breast) is very empty, it is interesting to combine a mastopexy with the fitting of a breast prosthesis
The procedure is performed under general anesthesia. Dr. Lucas, who was trained at the breast center of the CHUV (University Hospital of Lausanne), performs a scar starting around the nipples but hidden in the colored part of the areola, and sometimes vertical from the nipple to the submammary fold, then in grade II and III ptosis, it extends horizontally hidden in the submammary fold. The mammary glandular tissue is preserved as much as possible, unlike breast reductions, the mammary gland resected during the operation is sent for analysis, then a skin closure is performed, usually without a redon. Dr. Lucas reshapes the structure of the breast gland to fill the cleavage and restore volume in the upper breast.
Dr. Lucas uses biological surgical glue for the scar so that the patient can shower on the second day after the procedure. In general, the procedure is performed on an outpatient basis, without the need for hospitalization.
Results:
Time frame for final results:
2 weeks to see a significant result, 2 to 5 months to see the final result
Longevity of results:
Definitive, but with weight changes, pregnancies, breastfeeding and time, the breast will evolve.
Before surgery:
Stop smoking 1 month before surgery (risk of necrosis of the areola important if active smoking)
Do not take Aspirin 10 days before the operation, inform Dr. Lucas of any anticoagulant medication (Sintrom, Coumadin, Eliquis, etc.) in order to arrange for its discontinuation or replacement.
Take Arnica capsules 5 times a day for 5 days before surgery to prevent hematoma.
Shower with Hibiscrub soap provided on the prescription 48 hours before.
For patients over 35 years of age or if there is a family history of breast cancer, a screening mammogram should ideally be performed.
On the day of the procedure, you must not eat, drink or smoke for 6 hours beforehand.
Purchase before the procedure by you of a postoperative bra, the size of which will be specified to you by Dr. Lucas.
Procedure :
Duration of procedure: 90-120 minutes
Anesthesia: general
Location: operating room
Outpatient: no hospitalization, no redon
After surgery:
Post-operative pain: 1/10, with appropriate analgesia. Dr. Lucas performs an infiltration during the operation with long-acting anesthetics, in order to cover the 3 postoperative days.
Social eviction: 4-7 days with some discomfort. Shower possible from the 2nd day thanks to the use by Dr Lucas of biological surgical glue replacing the dressings.
Return to work: 10 days
Resumption of sports: 6-8 weeks
Instructions:
Arnica capsules 5 capsules 5 times a day for 5 days after surgery to prevent hematoma.
Stop smoking permanently to minimize complications.
Control Dr Lucas D2, D7, 3 weeks, 3 months, 6 months, 1 year
During the first 3 days especially: no rapid effort, rest, do not get up too quickly, take it easy so as not to make any sudden movements (efforts may increase the tension and open the small vessels and thus cause a hematoma)
Compression bandage around the breasts for 24-48 hours, then put in place during the consultation at 2 days of the support bra
Do not lift arms above 100°, do not carry heavy loads > 3-4 kg and do not push for 6 weeks.
Bra without underwire for 3 weeks day and night, 3 weeks during the day.
Shower from the 2nd day: pass water over the scar without rubbing, dab with clean cloth without rubbing
Between the 2nd day and the 7th day, disinfect the wound once a day with Merfen spray or another disinfectant spray.
From the 15th day, gently rub glue on the scar which will disappear over several days without tearing it off
Bath from 3 weeks depending on the evolution of the scar at 3 weeks.
Massage scar with Gorgonium 2 times 5 minutes per day for 3 months after the shower, from the 15th day.
Strataderm silicone once a day for 3 months, starting on the 15th day.
Sun protection with an index higher than 50 during the 6 months following the surgery.
Follow-up of the scar by Dr. Lucas for 1 year after the surgery is essential.
Complications
– Hematoma, seroma: a hematoma can occur especially during the first 48 hours. If it is significant, it is necessary to intervene again and evacuate it. During the first few days, it is necessary to rest and not to make any sudden movements in order to reduce the risk of hematoma.
– Localized skin necrosis, necrosis of the areola: the risk of this is greatly increased by smoking intoxication.
– Infection: fortunately rare, infection may require antibiotic treatment.
– Decreased sensitivity of the areola: often transient, full recovery is generally achieved after a few months.
– Asymmetry
– Abnormal, hypertrophic or even keloid scars: patients with dark skin, at risk of abnormal scars, must pay particular attention to the care of the scar with Gorgonium and Strataderm; follow-up remains essential
– Breast lift and breastfeeding: there are no consequences on breastfeeding, the patient can breastfeed after a breast reduction.
– Scar dehiscence and delayed healing (favored by smoking): sometimes there are small openings of the scar of a few millimeters, which can be healed with dressings usually without the need for reoperation. The follow-up by Dr. Lucas of the scar is essential.
Combinations and alternatives
A abdominoplasty can be combined in the same operation and a so-called “Mommy makeover” can be performed: i.e. a breast lift combined with an abdominoplasty.